My First Medical Mission
November 16, 2019 to November 23, 2019
Fundación de Lili Hospital
Cali, Colombia
In October, I volunteered my neuromonitoring expertise on a medical mission in Cali, Colombia. Candice, a friend with whom I worked alongside at Riley Children’s Hospital, called me just a little over a month before the departure date to offer me this incredible opportunity. They needed a last-minute additional IONM specialist to volunteer with Global Spine Outreach, and I eagerly obliged!
As the second-largest city in Colombia, Cali has three hospitals. Our team of 13 was paired with both orthopedic surgeons and neurosurgeons from the Fundación de Lili Hospital, which was ranked the third best hospital in Latin America by the América Economía magazine. Dr. Tony Rinella, an orthopedic surgeon out of Chicago, led the trip to Cali with fellow surgeons Amrit Khalsa, Ashish Patel, and Ryann Hoel. We also had several instrument representatives present: two that live and work in Cali, a student, a nurse, an incredible point-person, Melissa, and of course, the amazing Nicole who rounded out the two-person IONM team.
On Sunday, we spent the first full day in the clinic with patients who required surgery for scoliosis, and those who had already undergone surgery during a previous rotation. Nicole and I spent the majority of our time in the “fun room” with the younger patients, making sure they were happy while they waited their turn for examination.
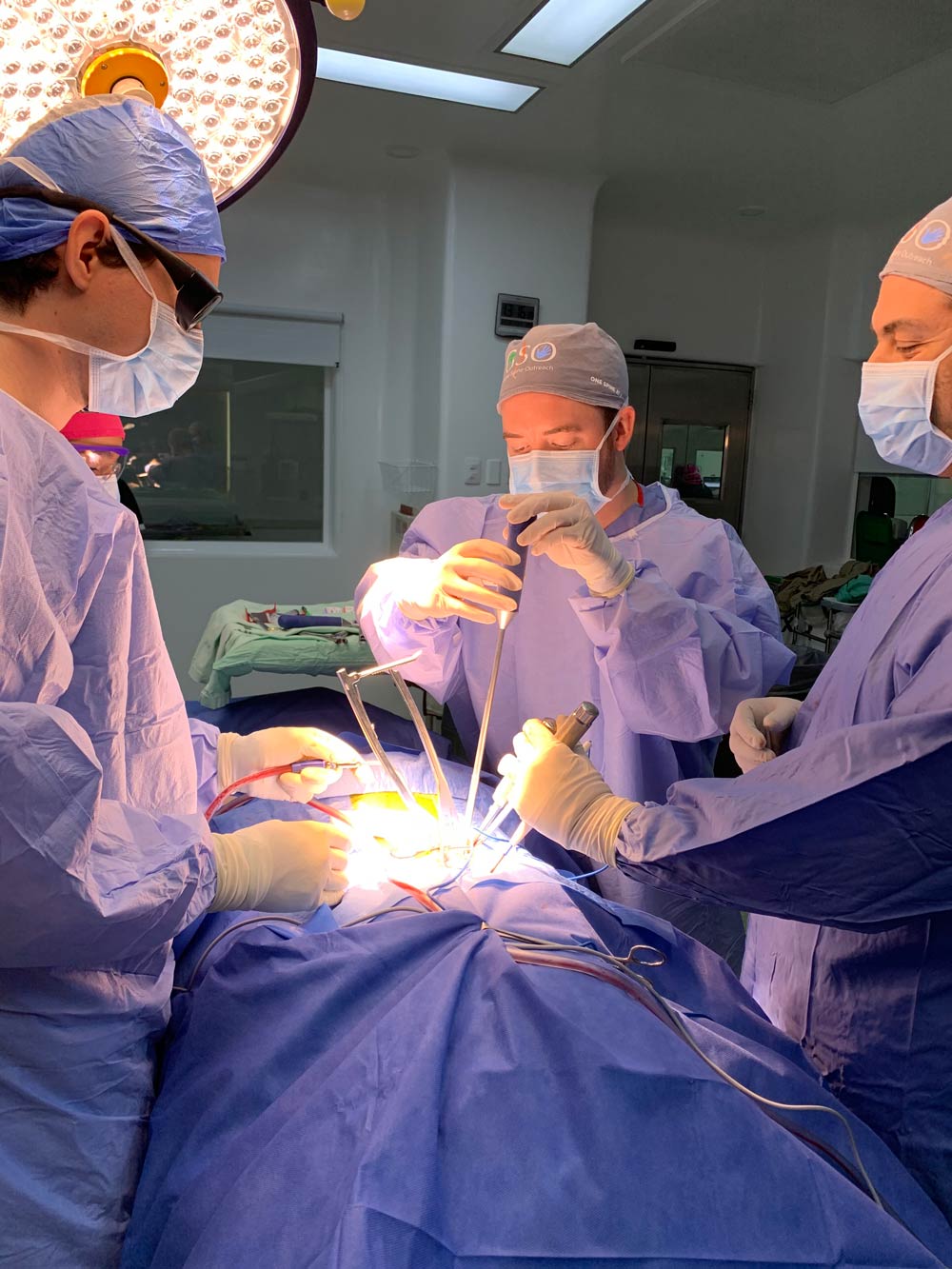
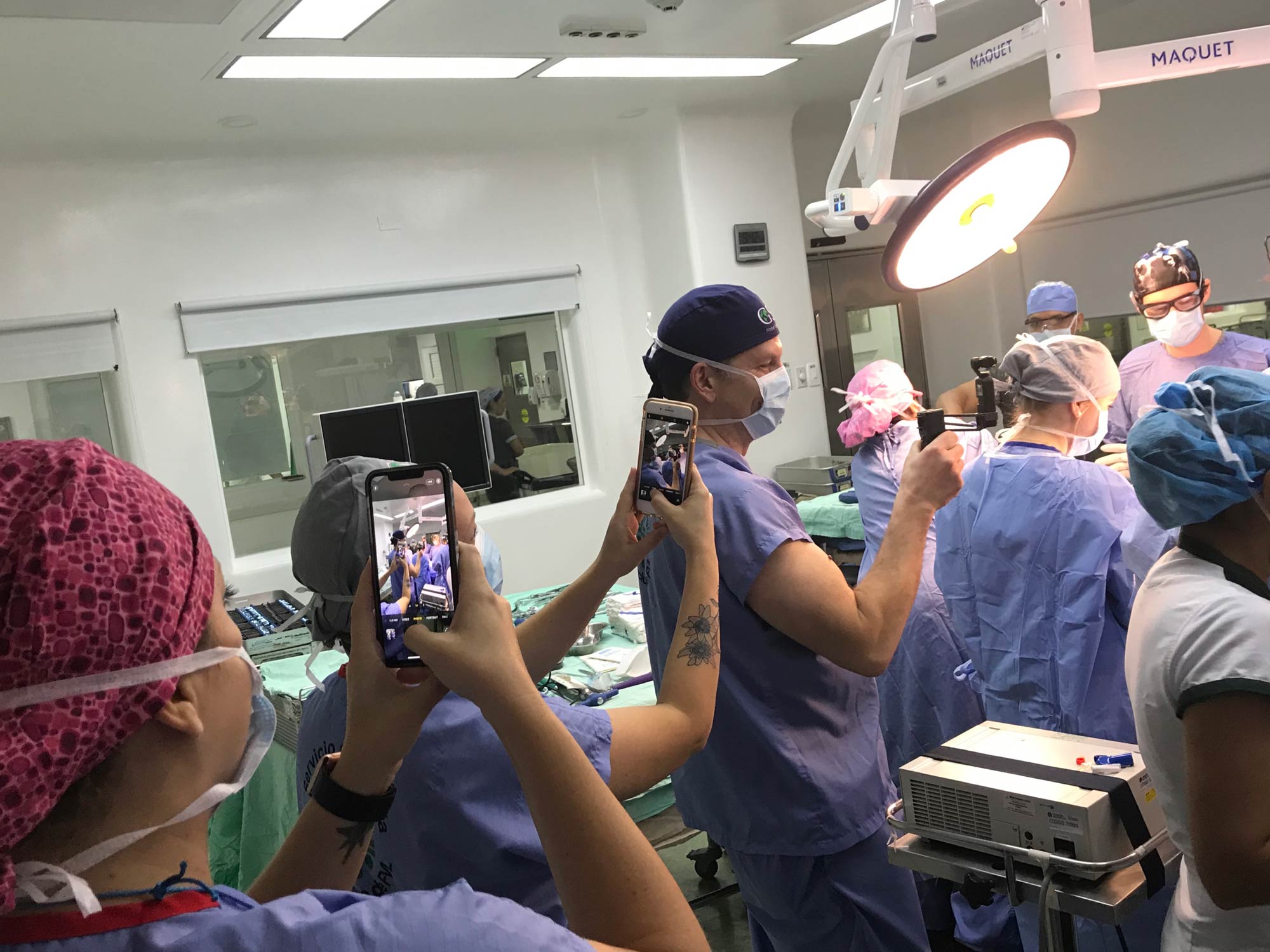
Over the next 5 days, we spent almost 80 hours in the operating room for 15 spine surgeries. We had 7 significant changes during our cases, and we monitored between 2 and 4 cases per day.
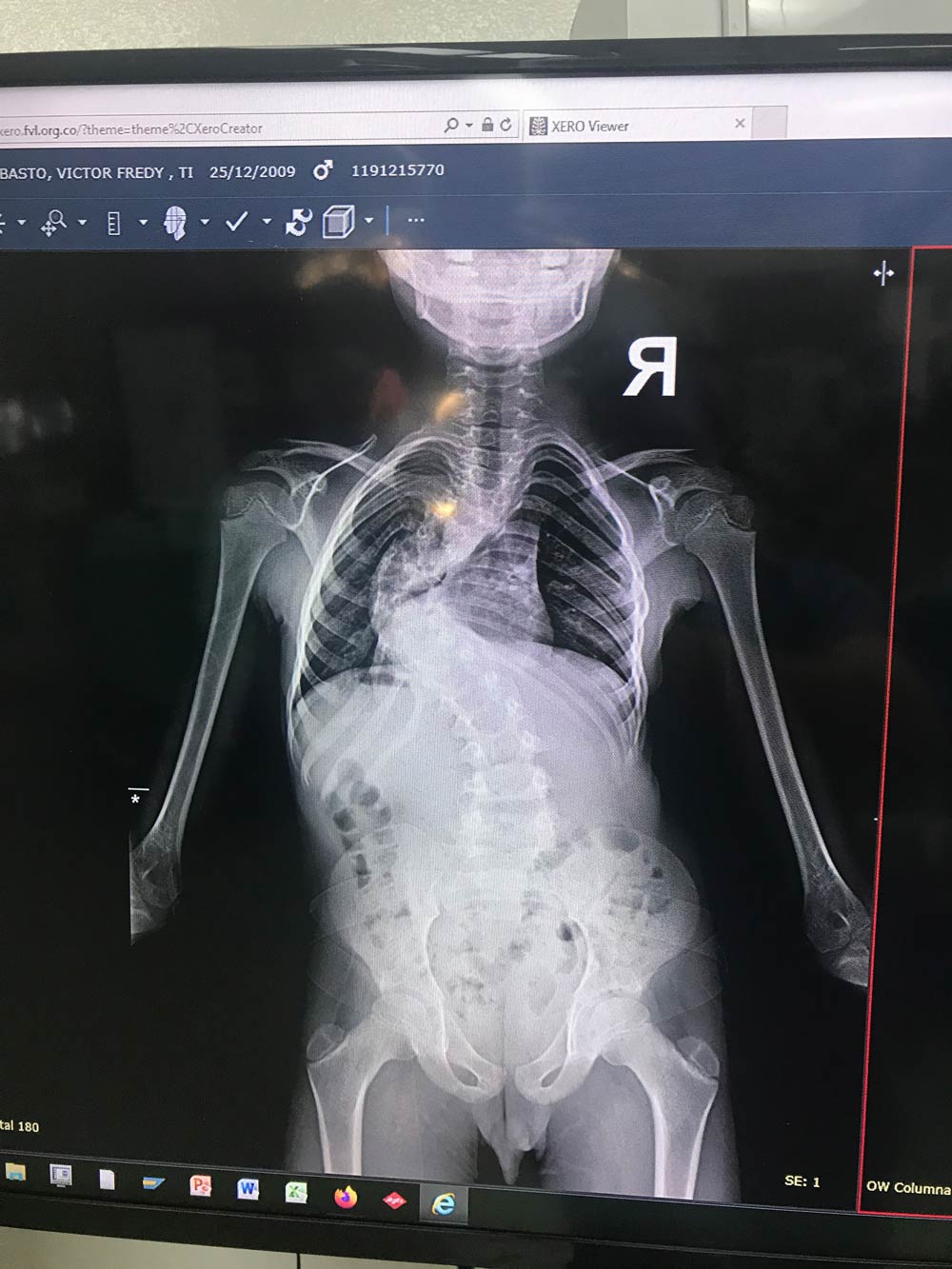
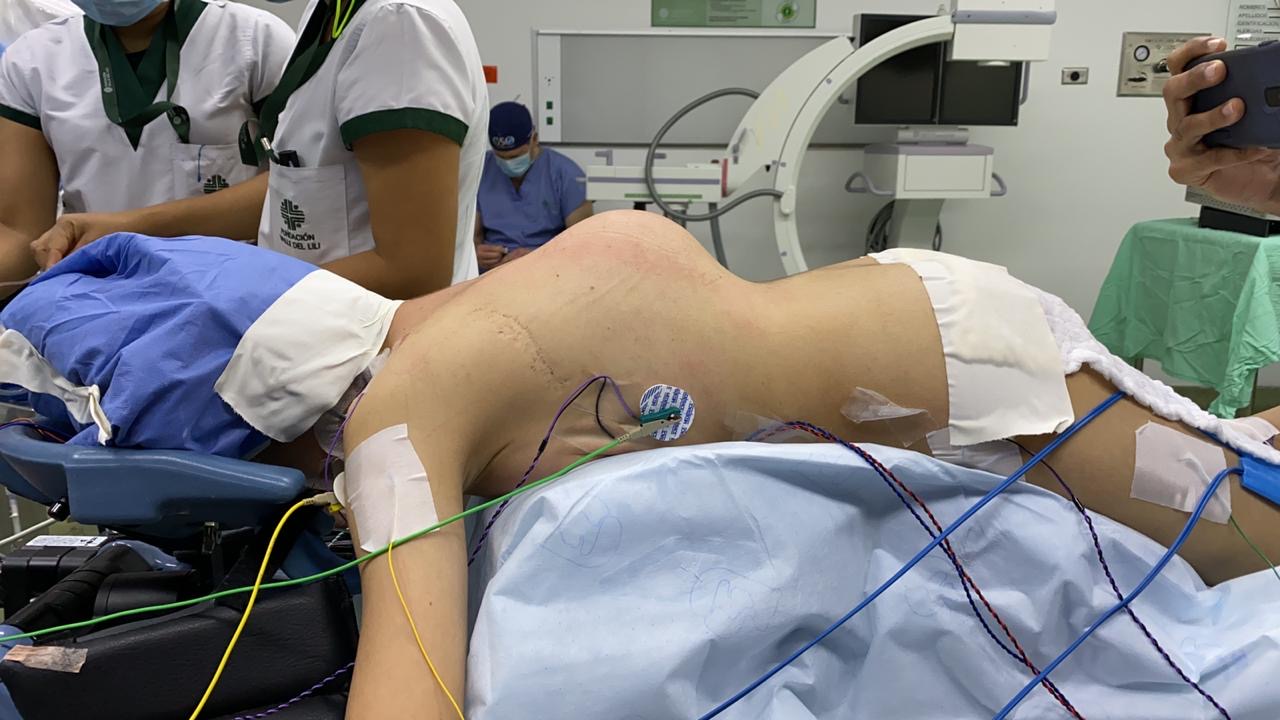
To introduce the sheer level of care, teamwork, and intraoperative complexity, I’ll touch on the craziness of the first day in the OR. My patient was a 14-year-old female with idiopathic scoliosis for a T2-L4 posterior spinal fusion. About 5 hours after a T7 screw placement, there was a loss of lower extremity corticals and total loss of motor responses below the T7 level. The screw was removed with no return; we stopped the procedure and closed. She moved both feet before leaving the operating room, and the surgeons staged her out for the remainder of the surgery, which was completed successfully with no further complications.
Nicole’s patient lost motors unilaterally after a T5 screw placement, and motors only returned after the screw was removed. The patient was a 20-year-old male with kyphoscoliosis for a T6 vertebral column resection and T1-L2 posterior spinal fusion. He lost motors again after rod placement, and his responses returned with rod adjustments. And to finish it out, after closing fascia, he coded with a pneumothorax and recovered nicely with a chest tube. Both patients were doing great when we saw them on the final day in recovery and post-op!
To say that day was emotionally taxing and exhausting would be an understatement. Collectively, we spent almost 20 hours in the operating room. The week didn’t slow down until Thursday afternoon, with only 4 growth rods to do on Friday. However, it turned out that Thursday was actually the most interesting day of the week. The entire country had scheduled a one-day national strike in opposition to the entire political setup in Colombia. The country’s major trade unions and the pseudo-left coalition Alternative Democratic Pole organized the strike which gained wide support and student groups also organized to strike independently. My patient was mid-screw placement on the second stage of my Monday procedure when all non-essential personnel were asked to leave the hospital. This was not only for safety reasons but also to ensure we could make the 7:00 pm curfew which had been imposed due to the strike. The GSO group stayed just long enough to place and secure the rods and we exited early, leaving the local orthopedic team to finish closing and remove 38 electrodes.
By the end of the trip, we had helped 15 children have the surgeries they needed to increase their quality of life and ease their pain. Our patients ranged in age from 9 to 20. Most of our cases were big fusions for scoliosis correction, an in situ fusion, several lengthenings, two vertebral column resections, some Magec rod placements and an Occiput to C3 posterior fusion for a 12-year-old patient with Morquio Syndrome. We monitored motor evoked potentials, electromyography with screw stim (intercostal muscles down to feet), and somatosensory evoked potentials on every patient. Our shortest surgery was 1 hour and 40 minutes, and our longest was 12 hours and 20 minutes.
This was my first experience volunteering for a medical mission, and it was one of the most meaningful things I’ve ever done. The group that Melissa and Candice organized was the definition of an A-Team, and we grew close over the trip. We spent the mornings at breakfast over coffee and each evening together as a group eating great Colombian food (and interesting pizza with plantain topping), drinking wine, and getting to know each other. To this day, we continue to message one another whenever inside jokes come up. The whole trip was incredibly rewarding for the entire team– and, more importantly, the effect it had on our patients and their families will last a lifetime.
Best,
Jim Leuck
Indiana Regional Director, Surgical Neurophysiologist